CARDIAC POCUS
To view the heart, we must look between the ribs and deep to the intercostal muscles, locating the heart just between the left lung and the sternum. Some hearts sit high in the chest, some lower, some more lateral, and some more medial. Some are deep inside the chest, and some are very superficial. Some are completely obscured by hyperinflated lungs, while others can be seen with perfect clarity. This page is a quick guide to the main POCUS views. For more in depth discussion and how to videos, considering getting a copy of The POCUS Textbook.
Cardiac POCUS Overview
Patient Positioning and Probe Selection
For some views, the patient can be supine to adequately visualize the heart. In most views, however, the image will be crisper if the patient can lie on their left side in the left lateral decubitus position. For cardiac ultrasound, you need to use the phased array probe, or a handheld ultrasound in the cardiac preset.
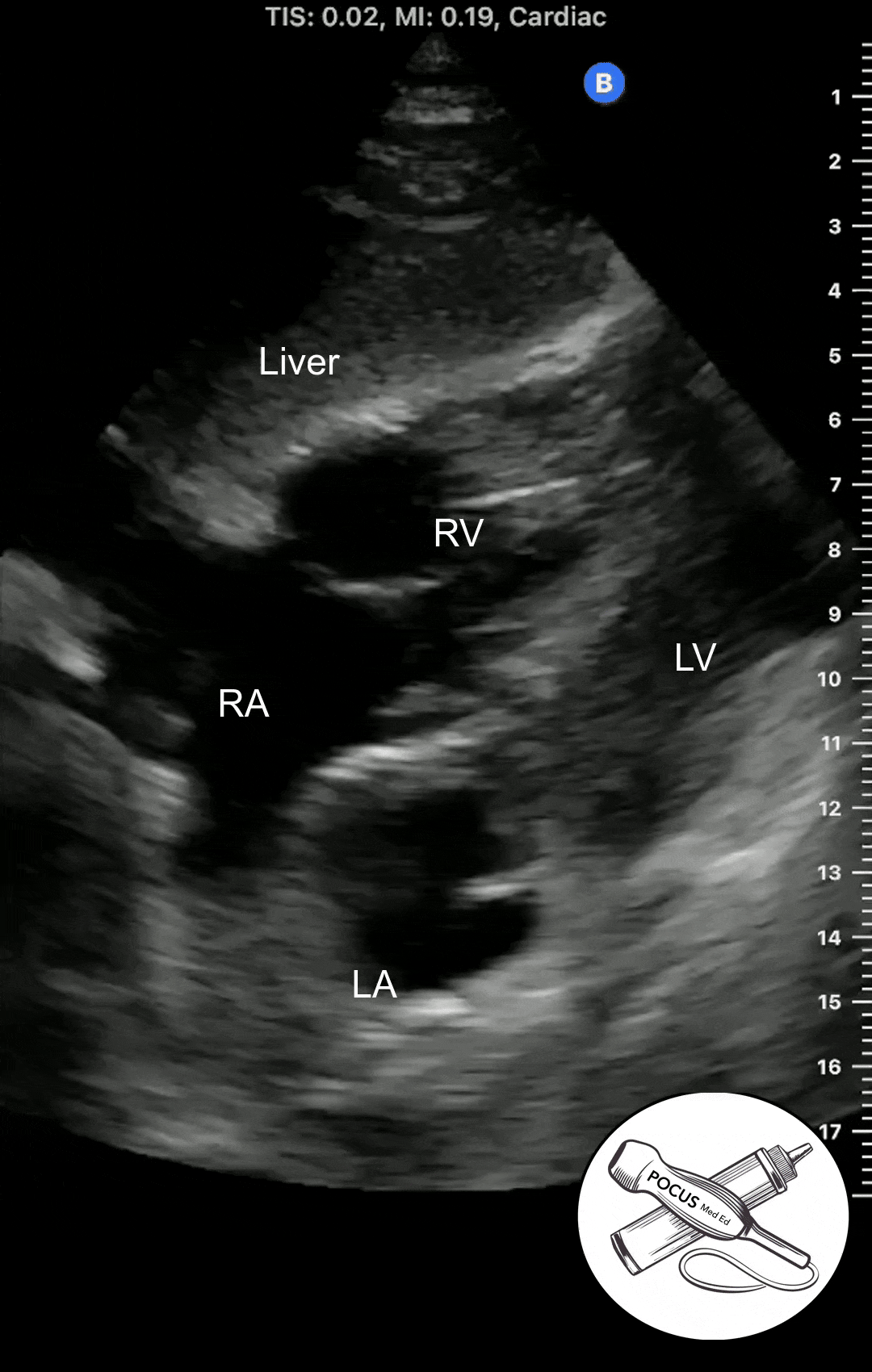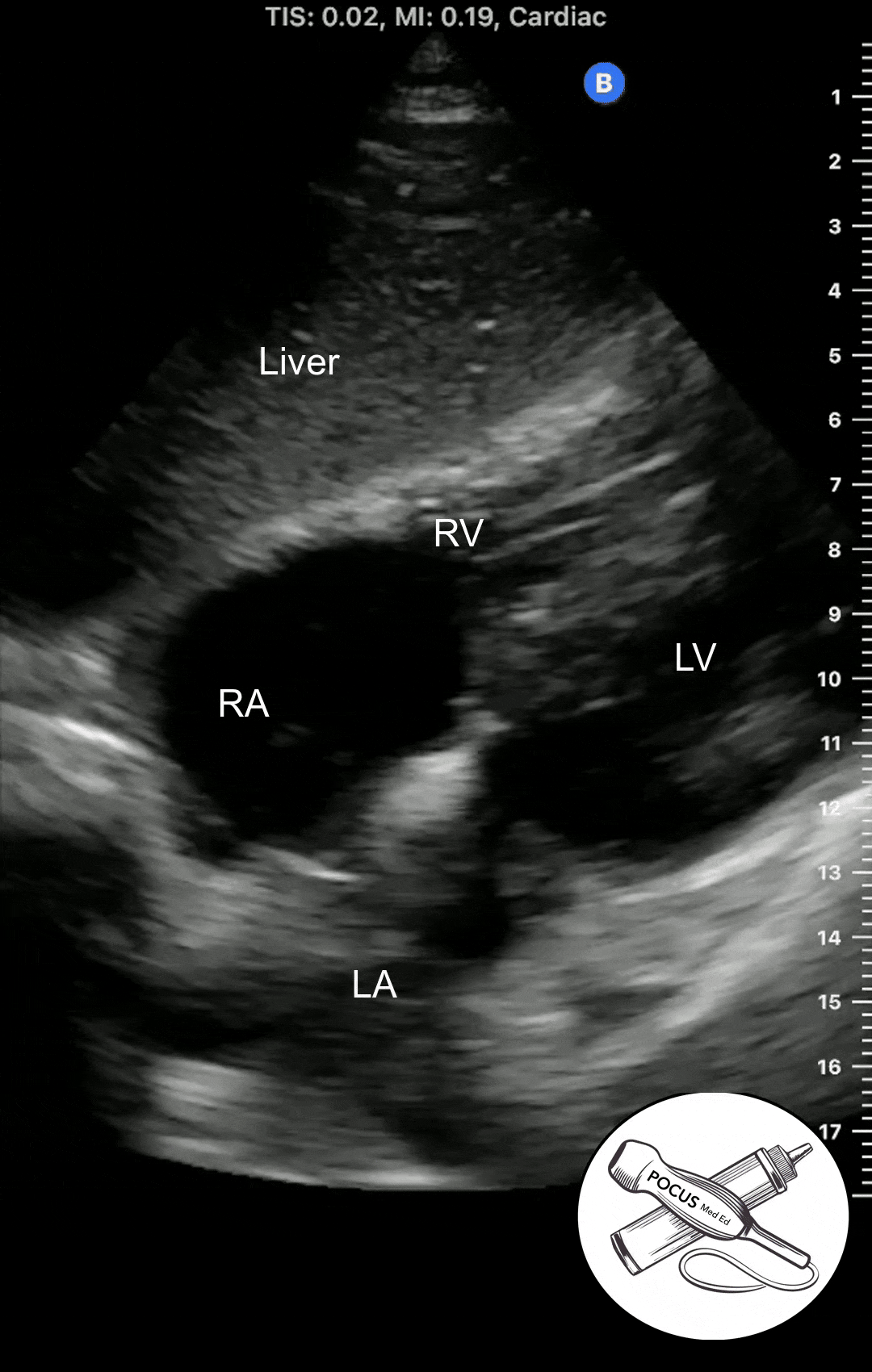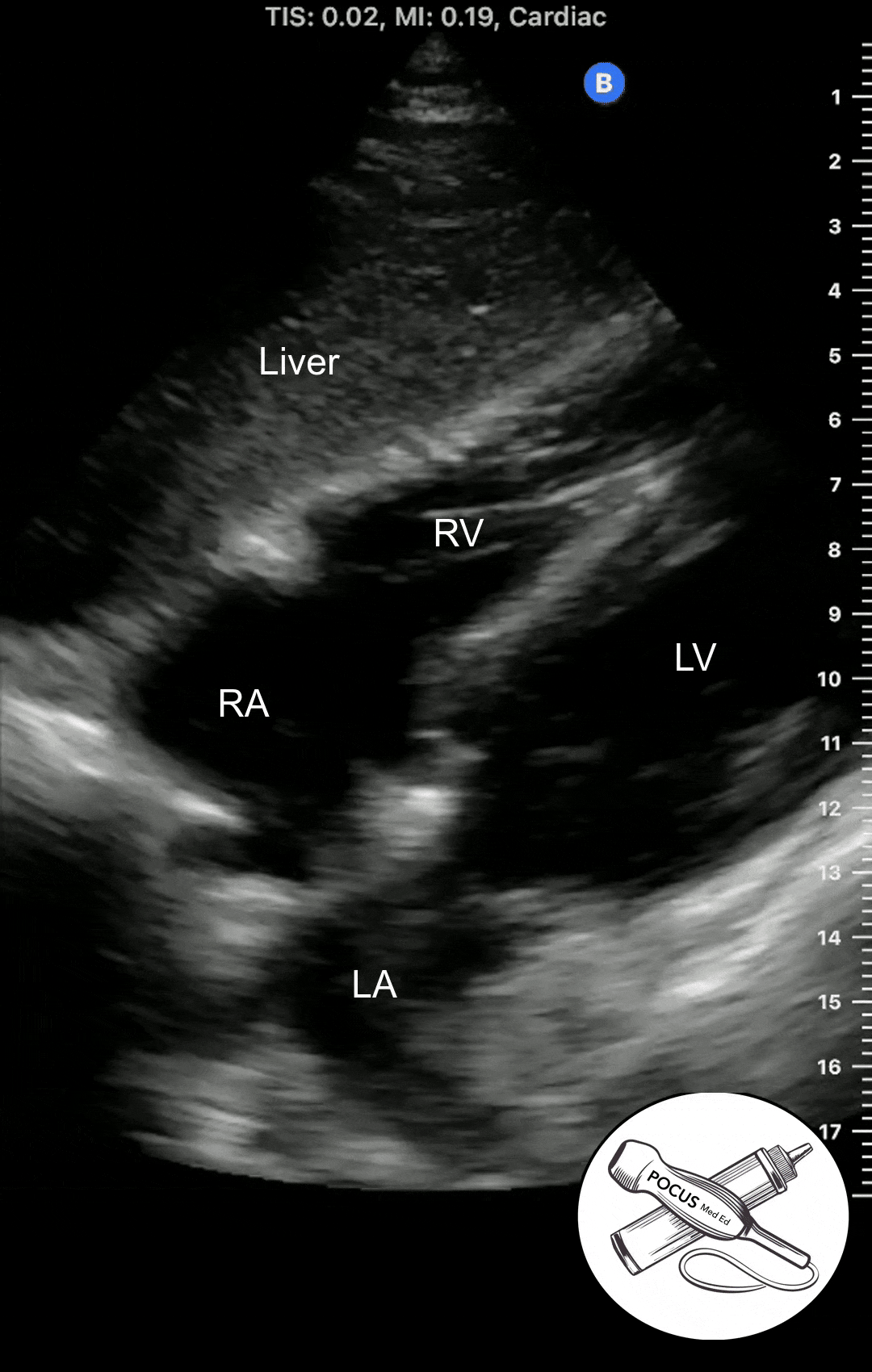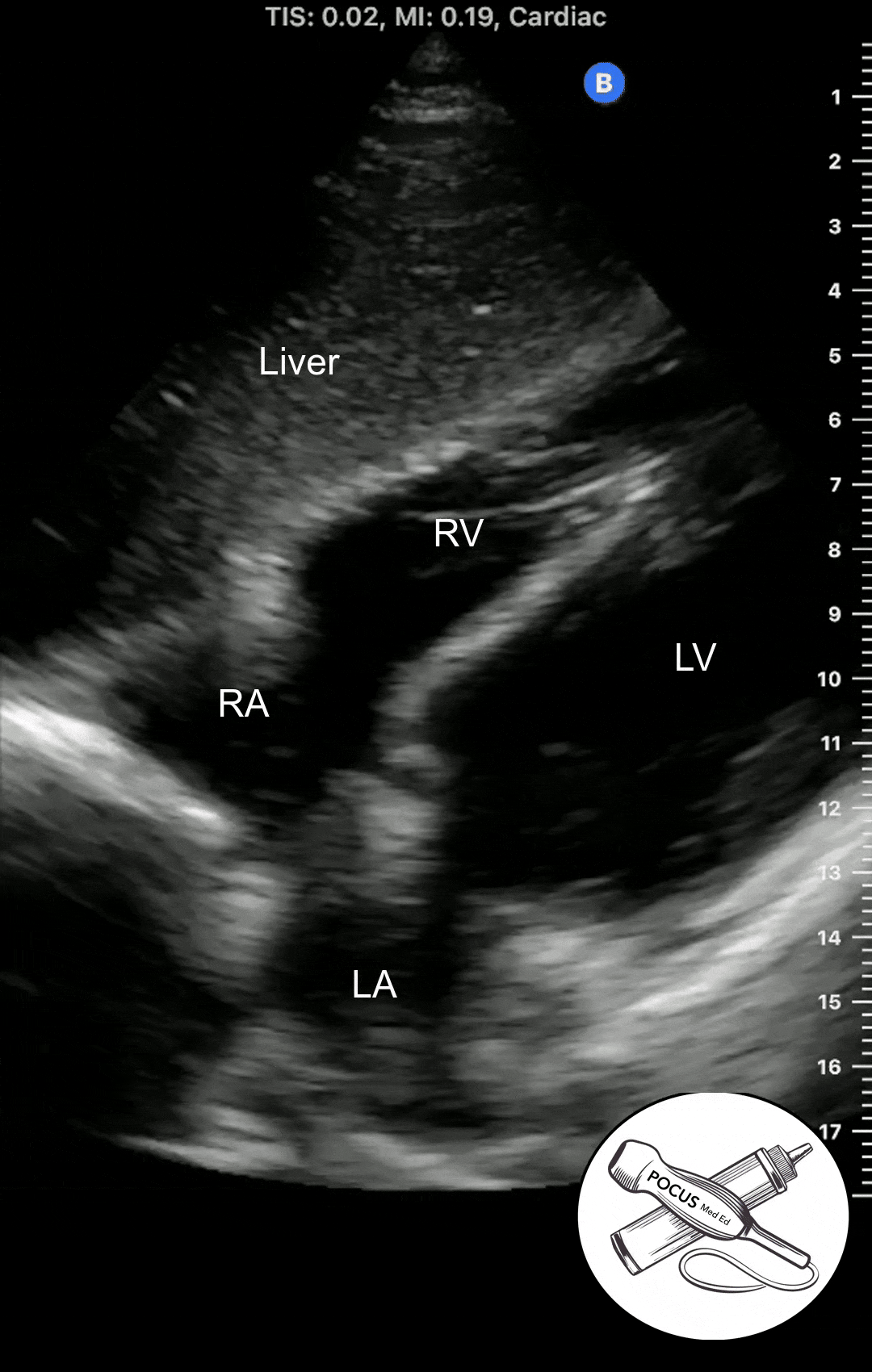
Parasternal Long Axis View
Place patient in supine or left lateral decubitus position. With the probe marker toward the patient's right bicep region, start high on the chest in the first or second rib space. Slowly sweep the probe down toward the feet, one rib space at a time until you reach the 3rd or 4th intercostal space.


The Parasternal Long Axis View is great for estimating the ejection fraction, screening for mitral or aortic regurgitation or looking for a pericardial effusion.
Parasternal Short Axis View
Once you have acquired a clear parasternal long axis view, rotate the probe 90 degrees so the probe marker is now facing the patient's left shoulder. You should now see a cross-section of the heart with the papillary muscles on either side.

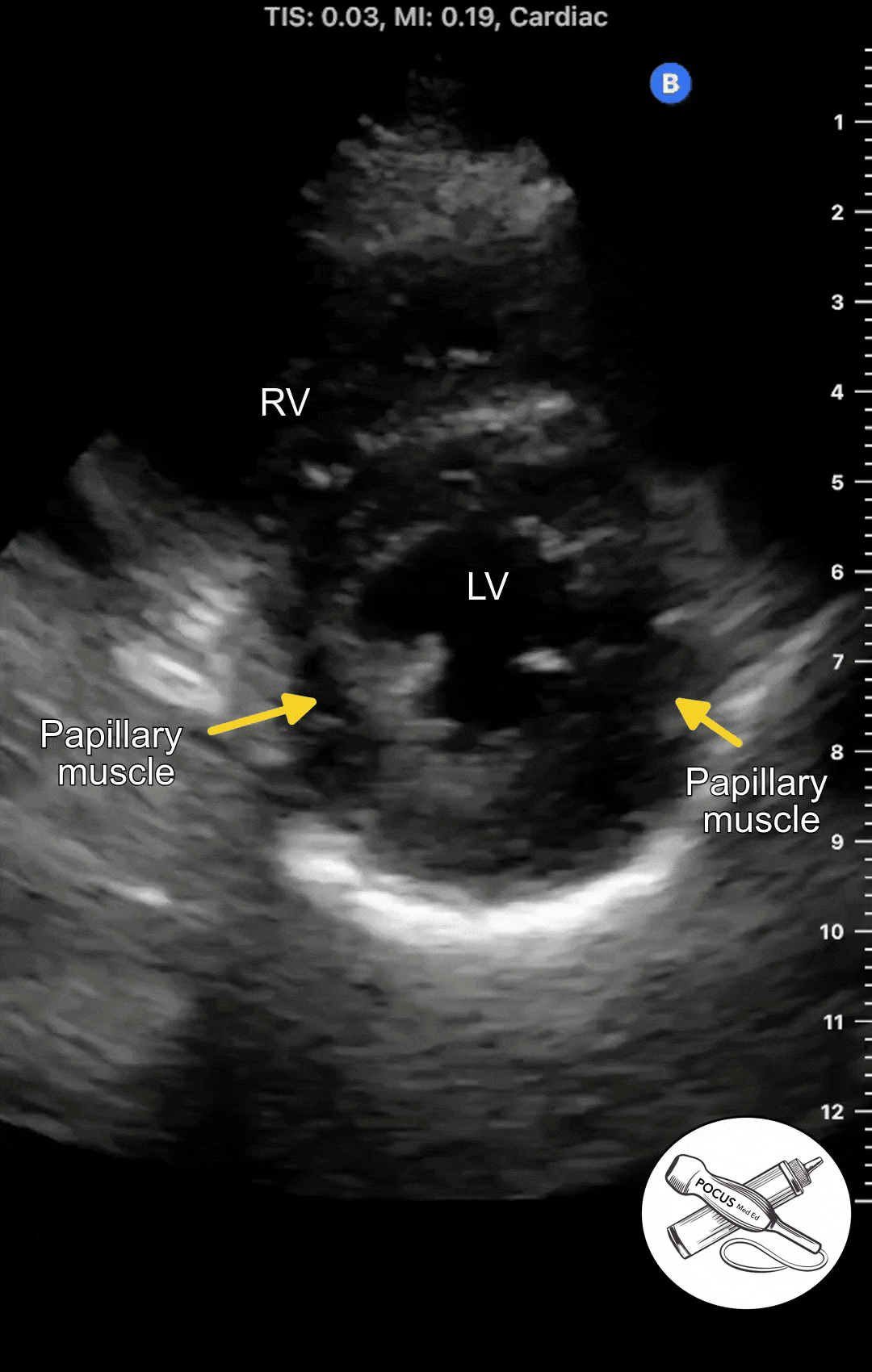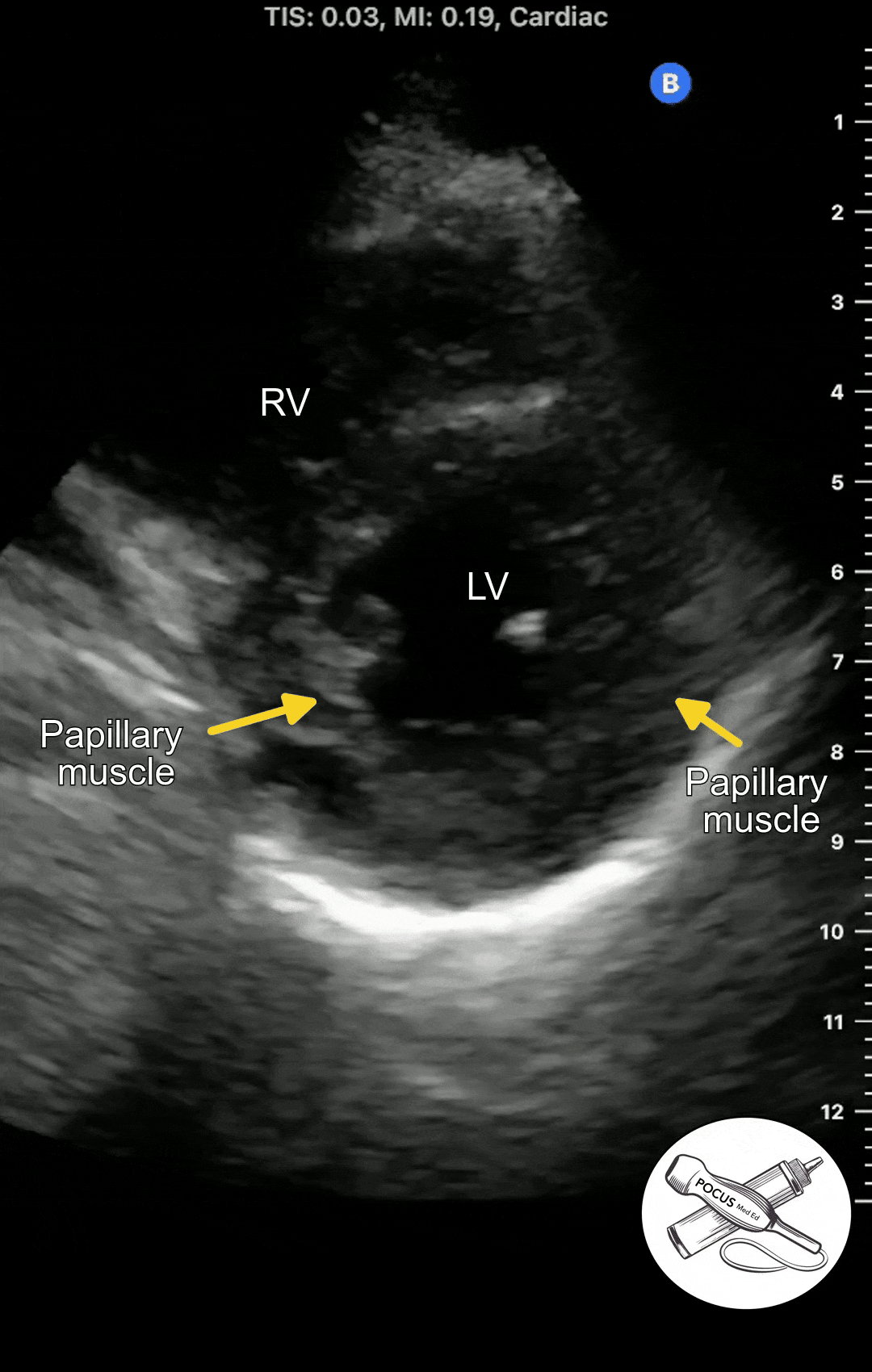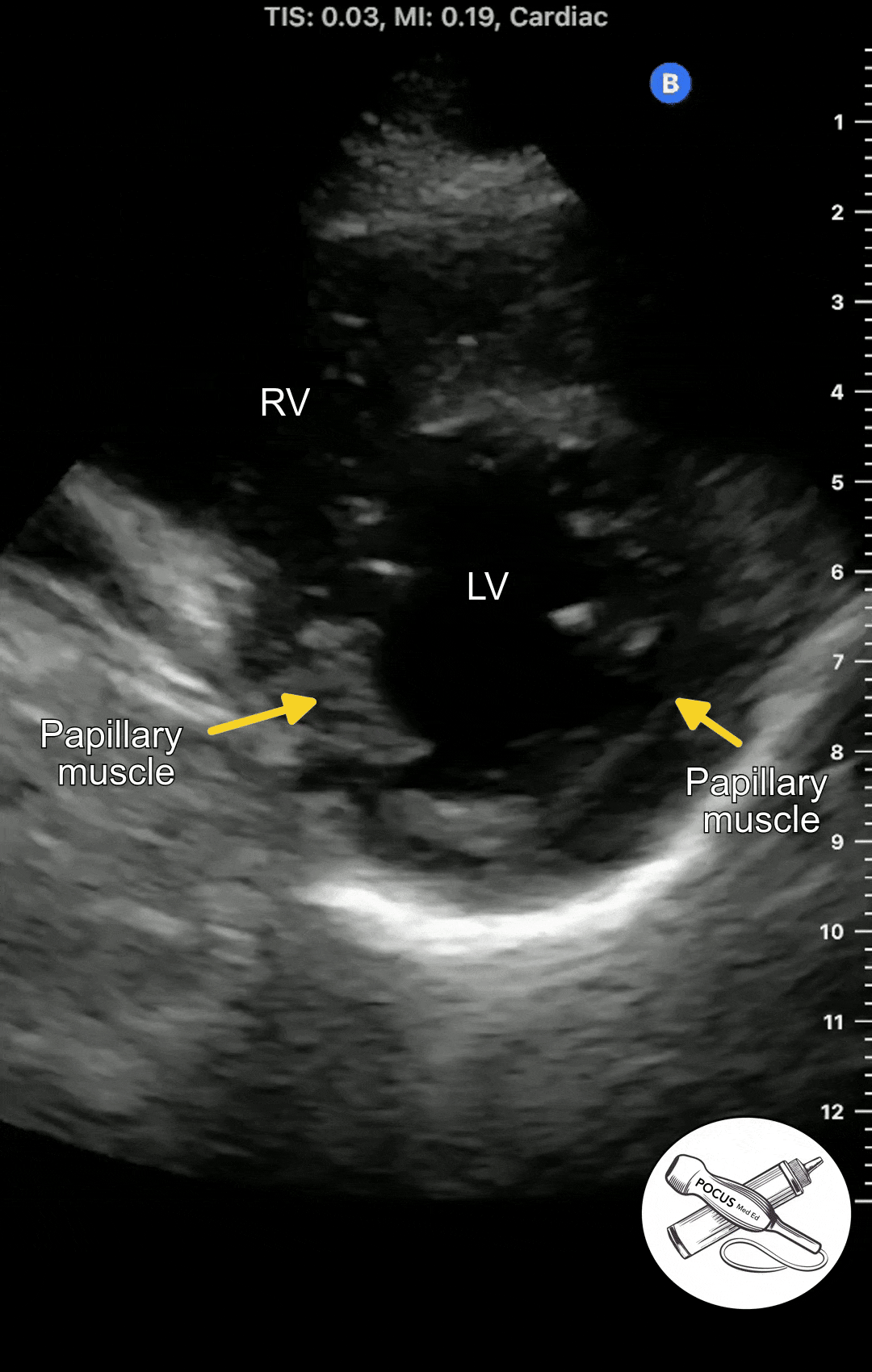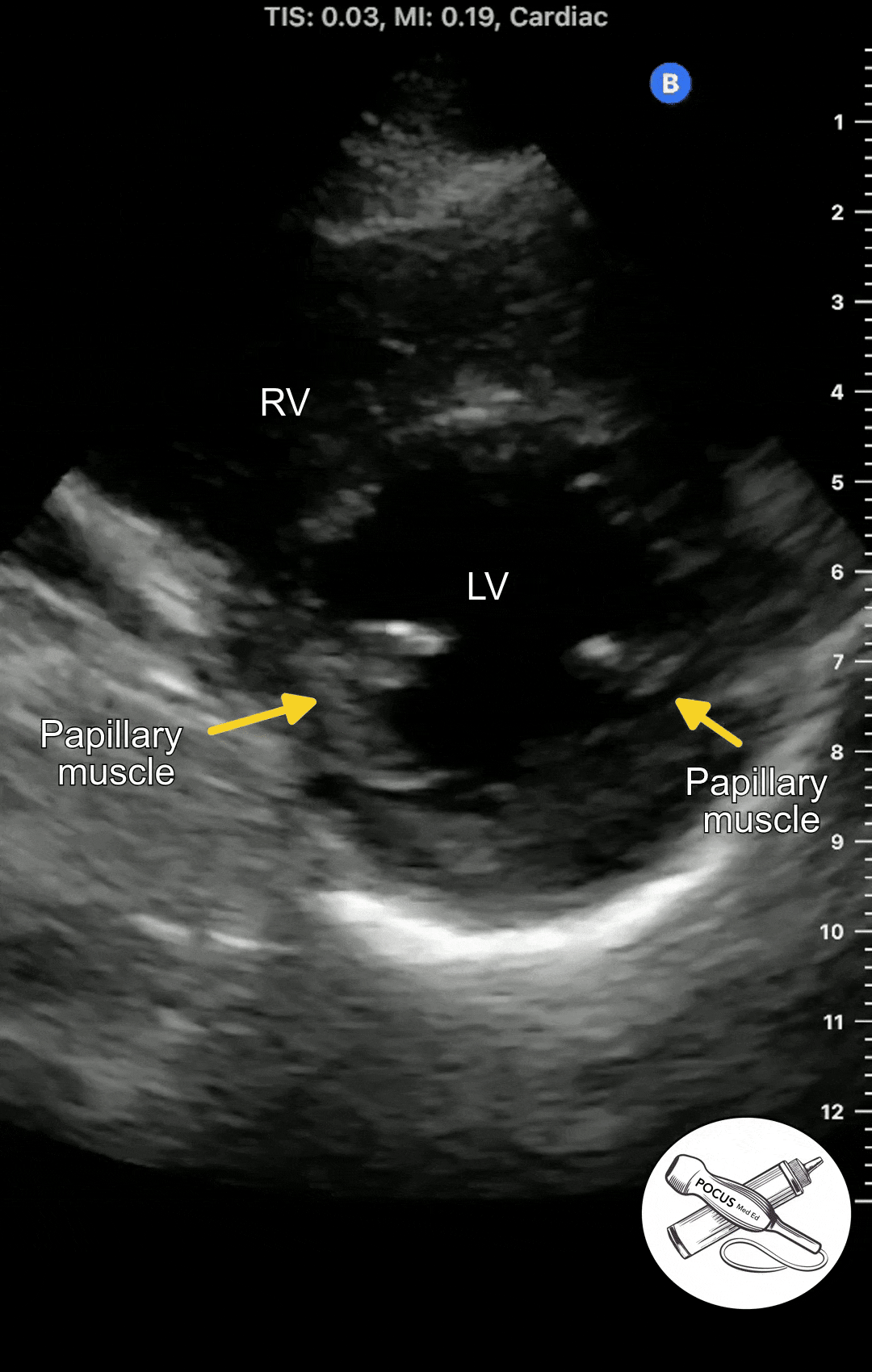
The Parasternal short axis view allows you to see a cross-section of the left ventricle. The ejection fraction can be estimated from this view. The symmetry or asymmetry of the left ventricular wall motion can be evaluated in patients with chest pain or shortness of breath. The right ventricle can also be seen. In normal conditions, It is crescent shaped and smaller than the left ventricle.
Apical 4 Chamber View
The Apical 4 Chamber View of the heart can be obtained in the Apical Window, which is usually in the inferolateral region of the chest. It looks at both the right and left heart from the vantage point of the apex. It can be difficult to acquire so it is important to optimize patient positioning and have a systematic approach.
To get an idea of where a patient's apex may be, first acquire a parasternal short axis view. Then tilt the probe down toward the patient's left flank until the left ventricular apex is visualized. Then place the probe in the inferolateral region in the approximate location of where the LV apex was seen in the parasternal short axis view.

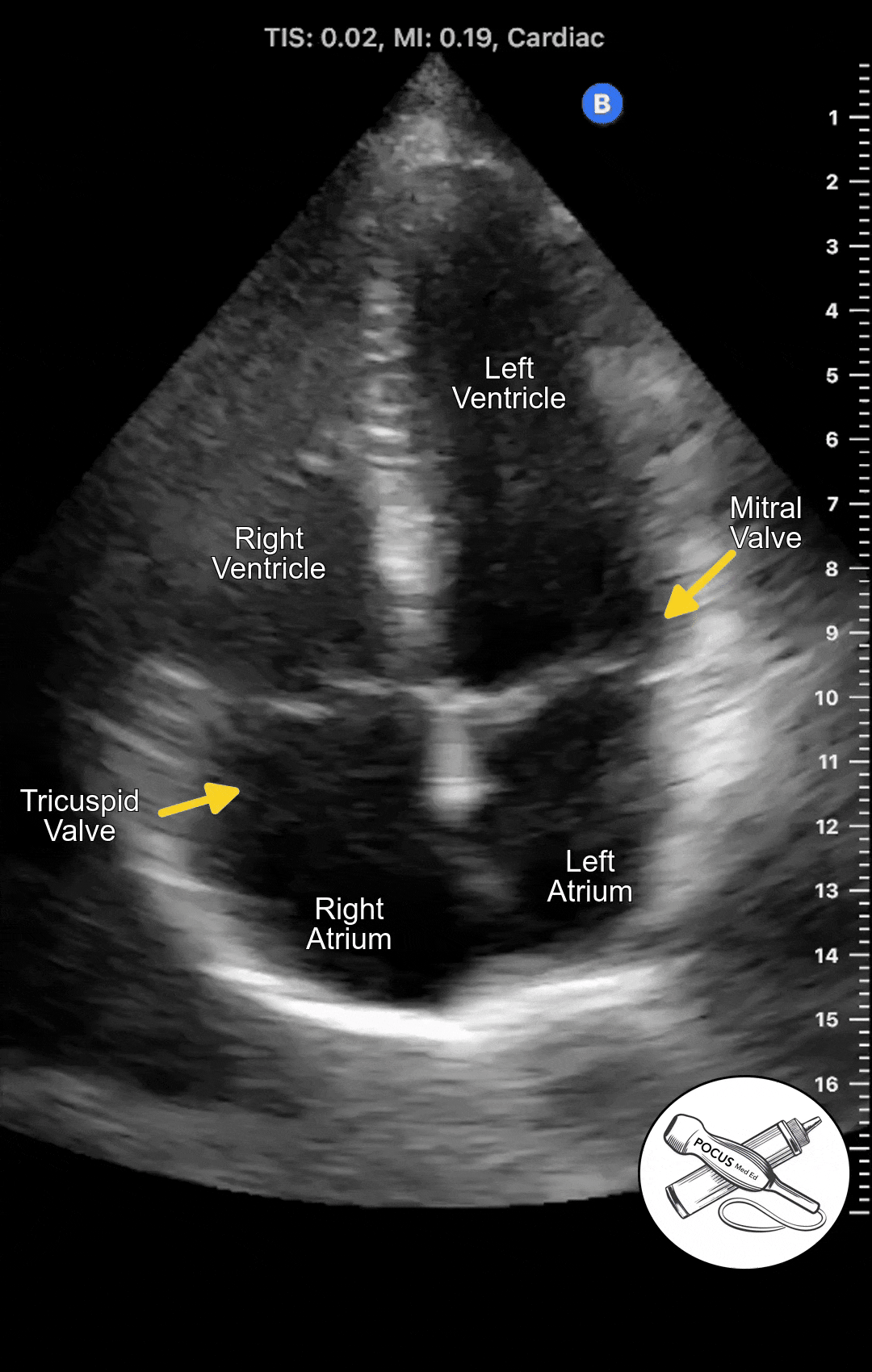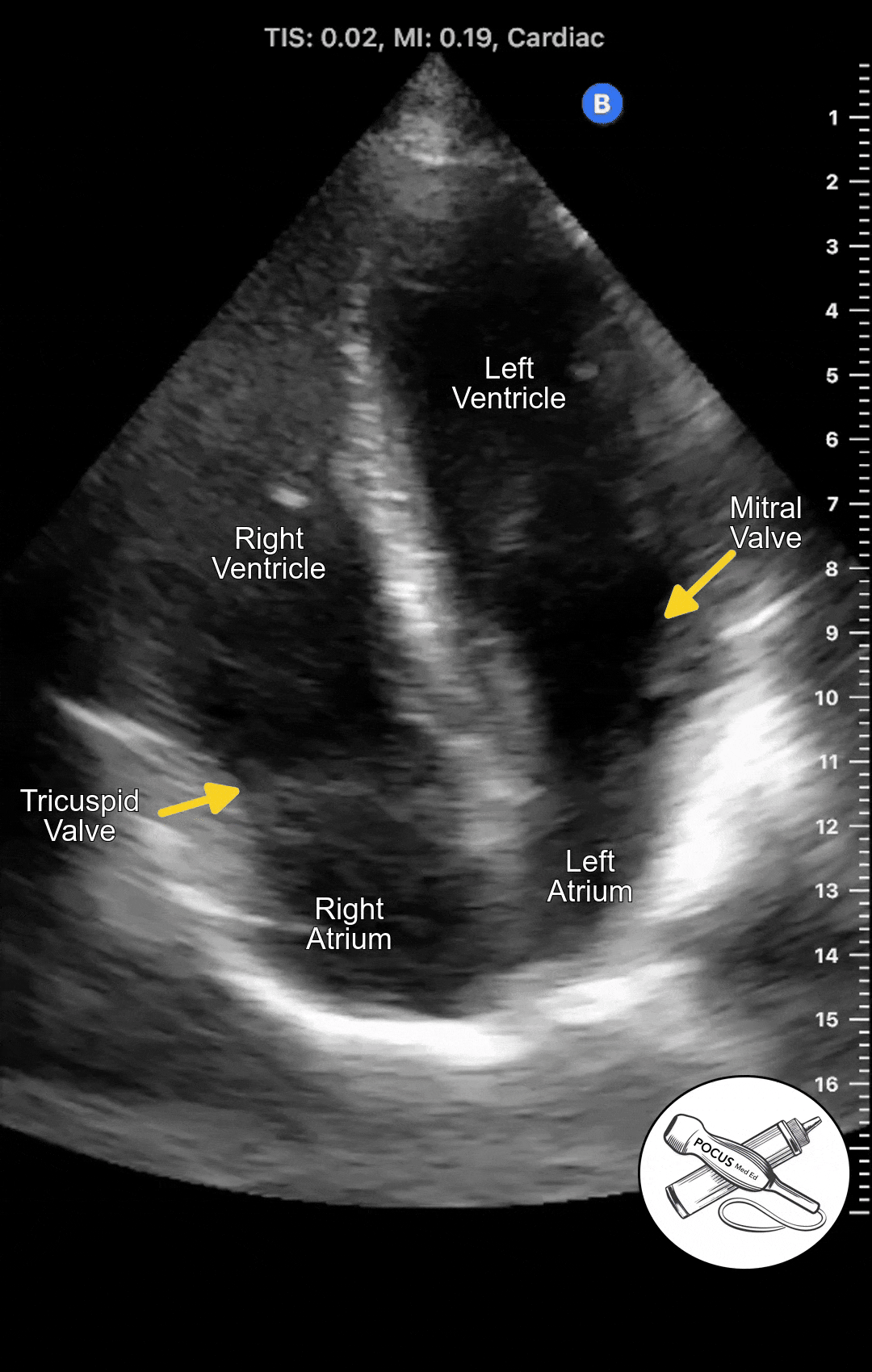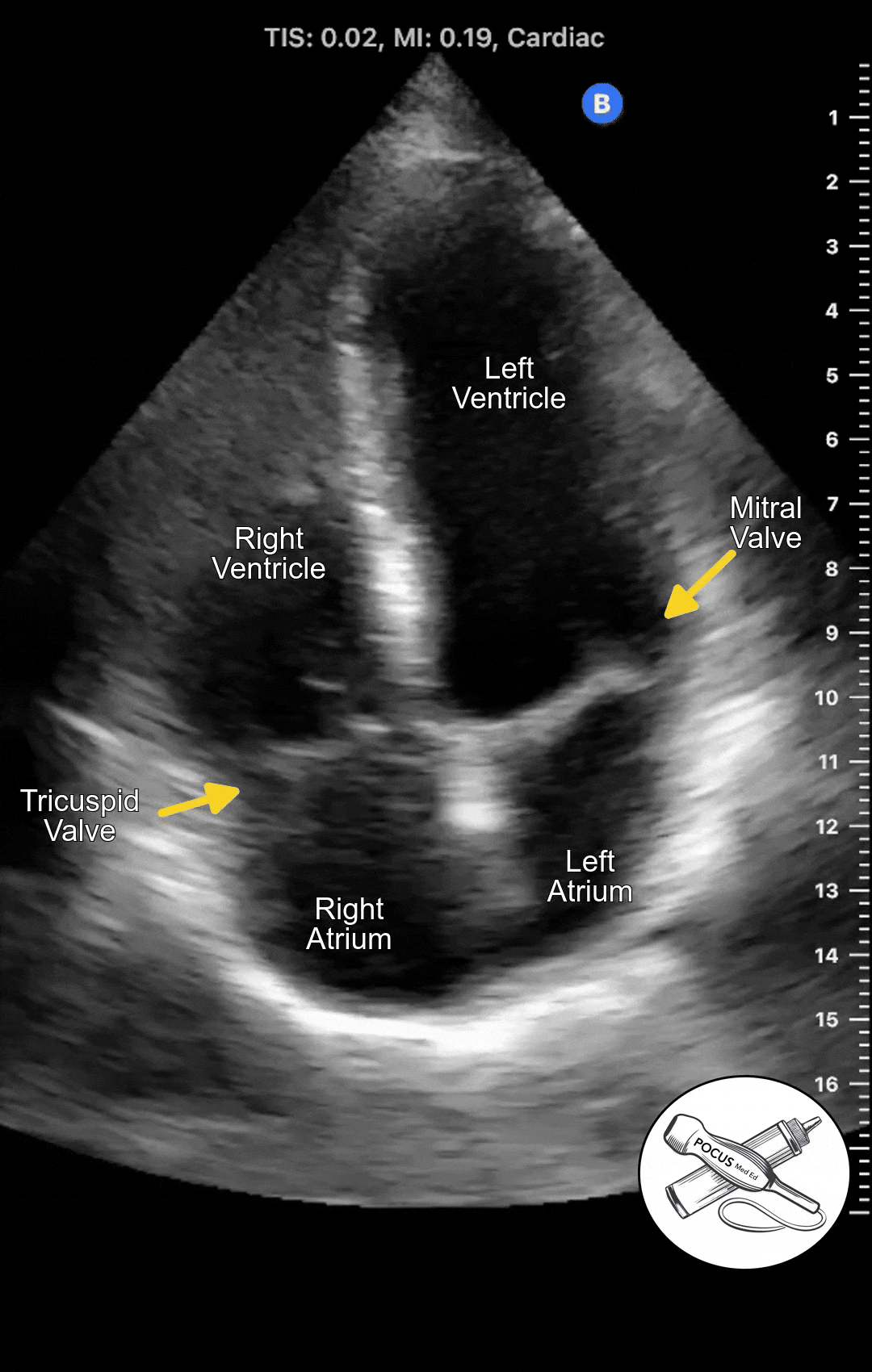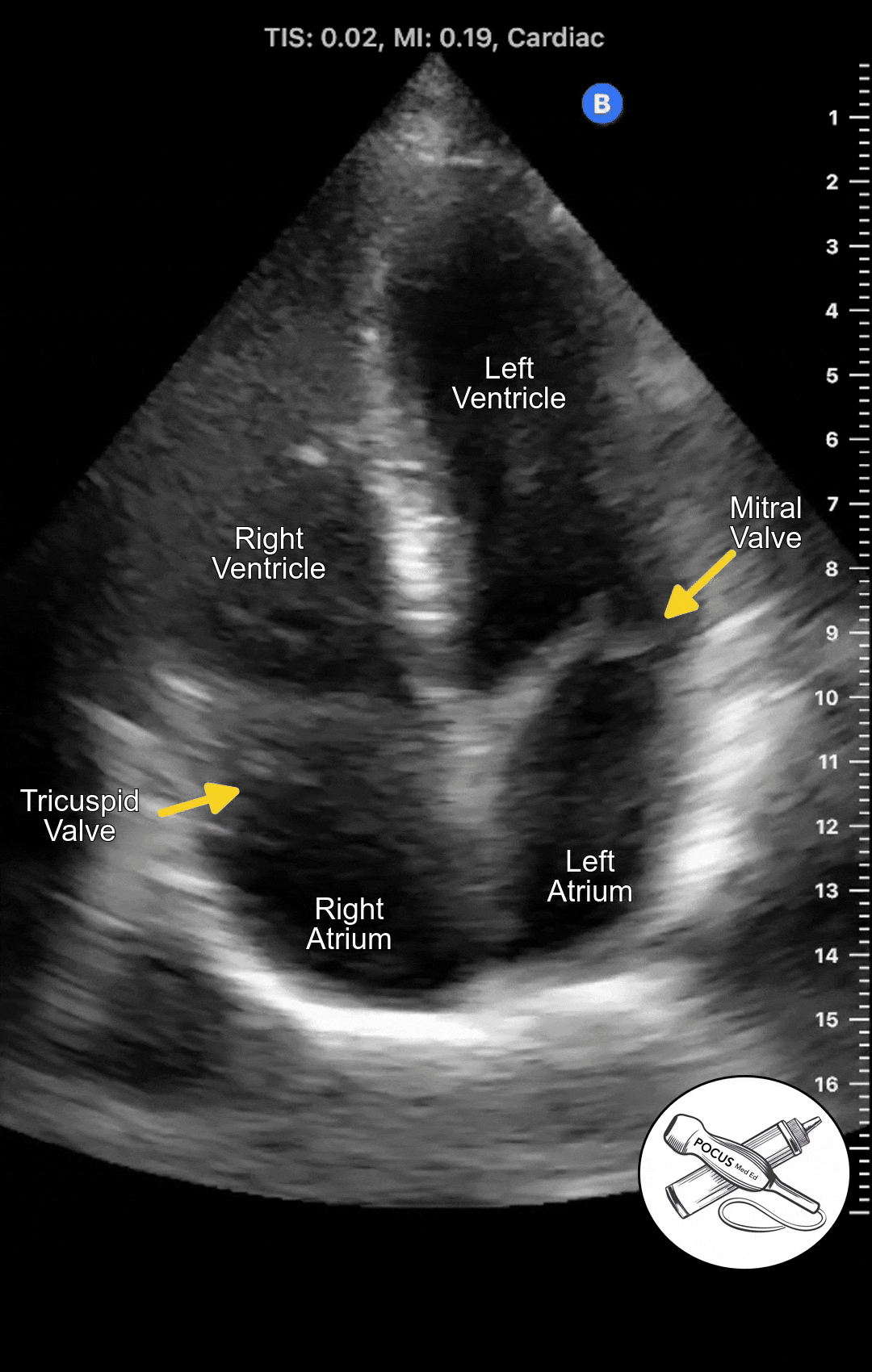
The Apical 4 Chamber View shows the ventricles and atria side by side. This view is best for evaluating wall motion and ejection fraction as well as visualizing the mitral and tricuspid valves. This is also the best view to screen for mitral or tricuspid regurgitation.
Subcostal 4 Chamber View
Once you have acquired a clear parasternal short axis view, rotate the probe 90 degrees so the probe marker is now facing the patient's left shoulder. You should now see a cross-section of the heart with the papillary muscles on either side.